Aortic coarctation in the wake of COVID-19 resulting into brain aneurysm in a Tanzanian patient, diagnostic and management dilemma: a case report
Reuben Kato Mutagaywa, Mark Mayala, Zalha Nuhu, Justus Ishengoma, Ally Qassim, Henry Mayala, Muhammed Bakari
Corresponding author: Reuben Kato Mutagaywa, Muhimbili University of Health and Allied Sciences, School of Medicine, Dar es salaam, Tanzania 
Received: 23 Mar 2022 - Accepted: 28 Jun 2022 - Published: 01 Jul 2022
Domain: Radiology,Cardiology,Neurosurgery
Keywords: Coarctation, aorta, aneurysm, refractory hypertension, COVID-19, case report
©Reuben Kato Mutagaywa et al. PAMJ Clinical Medicine (ISSN: 2707-2797). This is an Open Access article distributed under the terms of the Creative Commons Attribution International 4.0 License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Cite this article: Reuben Kato Mutagaywa et al. Aortic coarctation in the wake of COVID-19 resulting into brain aneurysm in a Tanzanian patient, diagnostic and management dilemma: a case report. PAMJ Clinical Medicine. 2022;9:19. [doi: 10.11604/pamj-cm.2022.9.19.34445]
Available online at: https://www.clinical-medicine.panafrican-med-journal.com//content/article/9/19/full
Case report 
Aortic coarctation in the wake of COVID-19 resulting into brain aneurysm in a Tanzanian patient, diagnostic and management dilemma: a case report
Aortic coarctation in the wake of COVID-19 resulting into brain aneurysm in a Tanzanian patient, diagnostic and management dilemma: a case report
Reuben Kato Mutagaywa1,2,&, ![]() Mark Mayala1, Zalha Nuhu1, Justus Ishengoma1, Ally Qassim2, Henry Mayala3, Muhammed Bakari1
Mark Mayala1, Zalha Nuhu1, Justus Ishengoma1, Ally Qassim2, Henry Mayala3, Muhammed Bakari1
&Corresponding author
Aortic coarctation is a congenital disorder of the aorta. Symptomless refractory hypertension can be its only presenting form, resulting into its late diagnosis and subsequent complications. A case report of a 19-year-old male with a late diagnosis of secondary hypertension due to coarctation of the aorta (CoA) complicating to aneurysm of basilar tip is presented. The patient was apparently well until when he presented with palpitations and intractable headache at the age of 14 years. Over a period of 5 years he was being treated as a patient of hypertension in the health facilities at the peripheral, despite of non-response to treatment. Upon arrival at the tertiary level hospital (Muhimbili Orthopedic Institute) on 14th June 2021, the investigations were done and confirmed a diagnosis of CoA and aneurysm of basilar tip. Until 8th June 2022 he is on medical treatment but without control of the blood pressure. The patient is waiting for interventional treatment, preferably percutaneously, but this service is not available in the country due to the absence of interventional equipment. The plan is to refer the patient to abroad. However, he is not capable of paying for himself and the current supporter is yet to decide on whether to cover the anticipated costs or not. The other option is to secure support from the government. Unfortunately, all these plans were further frustrated by travel restrictions which were imposed due to the COVID-19 pandemic. We obtained the consent from the patient to publish this case. The presentation of this case underscore on the importance for doctors at all levels of health facilities to always take into consideration the possibility of secondary hypertension in the young who presents with refractory hypertension, and that a correct physical examination must be conducted. In addition, challenging management issues in the resource-constrained setting and the COVID-19 pandemic have been discussed.
Coarctation of the Aorta (CoA) accounts for 0.1% of patients with secondary hypertension [1]. The condition is common in males, and can easily be suspected by proper clinical examination that includes measurement of blood pressures and palpation of femoral pulses. Rarely, CoA can present in adults as refractory hypertension 2]. Hence, failure to perform a thorough cardiovascular examination could lead to a late diagnosis and consequent serious complications [2]. The first surgical intervention for this disease was done by Dr. Crafoordin in the year 1944 [3]. Before that, CoA had a very poor prognosis with a median survival age of mere 31 years [4]. Subsequently, in early 1980s Transcatheter Balloon Angioplasty was introduced for management of CoA by Singer et al. [5] and later in the decade Transcatheter Endovascular Stent Therapy was introduced [6]. With these developments, the natural history of this disease has significantly improved allowing most patients making it to adulthood. However, availability of such interventions in most developing countries, including Tanzania, is restricted by lack of expertise, equipment and financial resources to cover for the cost of treatment. We report herein a late diagnosis of CoA as a cause of secondary hypertension in a 19-year-old male, which complicated to an aneurysm of the basilar tip, whose further management has also been hindered by the COVID-19 pandemic.
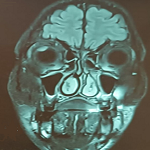
Patient information: a 19-year-old male, high school graduate, non-insured, non-alcoholic, non-smoker presented to a Neurosurgery Department of the Muhimbili Orthopedics Institute (MOI) as a referral case from a specialized polyclinic unit in Dar es Salaam with a diagnosis of brain aneurysm through CT scan Brain with contrast (Figure 1). The CT scan was done after he presented with a 3-year history of recurrent episodes of severe headache which worsened with time, was not relieved by painkillers, and was not associated with fatigue and sweating.
Timeline: he was diagnosed with Hypertension for 5 preceding years, and unfortunately this was not regarded as secondary. Despite being on antihypertensive medications for 4 years in the lower level facilities, good control of his blood pressure was never achieved. He had no personal or family features suggestive of chronic diseases like hypertension, diabetes mellitus or polycystic kidney disease. At a specialized polyclinic he was re-initiated on antihypertensives (Amlodipine, 10�mg, orally given twice daily; Carvedilol, 12.5�mg, orally, given thrice daily; Losartan/Hydrochlorothiazide, 65.2�mg, orally, once daily). He was on this regimen for 2 months and had good compliance, but there was no marked success in blood pressure control, and the headache persisted.
Clinical findings: on proper clinical examination at the Tertiary facility (MOI) it was found that although the femoral pulses were palpable bilaterally, they were weak. A brachial-femoral pulse delay was noted. The BP was 183/122 mmHg in the left arm and 130/115 mmHg in the left leg, with an ankle brachial index of 0.9. He also had an apical heave. Coarctation of the aorta was thus suspected, and further investigations were performed.
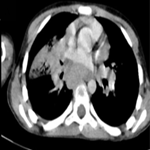
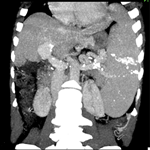
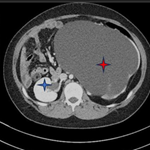
Diagnostic assessment: blood chemistry and urinalysis were normal. Marked rib-notching was revealed on chest X-ray (Figure 2). A Twelve-leads electrocardiogram revealed left ventricular hypertrophy (LVH), while a two-dimensional (2D) echocardiography (ECHO) confirmed the LVH with a normal left ventricular ejection fraction of 72%. The parasternal long-axis and short-axis views showed a tricuspid aortic valve with normal excursions. The transthoracic ECHO in suprasternal view showed an increased peak flow velocity of 3.5 m/s, indicating severe stenosis of the descending aorta. The computed tomographic angiography (CTA) showed severe coarctation of the aorta below the origin of the left subclavian artery, together with post stenotic dilatation (Figure 3). Numerous collaterals were also observed, as reported in Figure 4.
Therapeutic intervention and follow-up and outcomes: he was then referred to cardiothoracic surgery and interventional radiology to evaluate his candidacy for surgical or percutaneous therapy, of which percutaneous therapy was preferred over surgery. Currently, he is waiting to undergo percutaneous angioplasty with aortic stenting as well as digital subtractive angiography (DSA) with basilar tip aneurysm stent-assisted coil embolization. Unfortunately, the needed consumables are not available in our setting, so the patient has to be referred to abroad for further management. However, this is also a challenge as the patient is not insured (currently being helped by a private sponsor), and the COVID-19 pandemic was making travelling difficult. His proper management is therefore significantly hindered, putting him at an even higher risk for the aneurysm to rupture. He is thus still on antihypertensives (Amlodipine, Carvedilol, and Losartan/Hydrochlorothiazide) while waiting for the procedure. However, his blood pressure is erratically controlled. He was lastly seen at our clinic on 8th June 2022.
Patient perspective our patient reports that he is satisfied with the care and treatment he is receiving MOI, and he is hoping that he will receive a definitive treatment of his ailment soon.
Ethics declaration and consent for publication: ethical approval was not applicable. Written informed consent was obtained from the patient for publication of this case report and any accompanying images.
Coarctation of the Aorta is a congenital vascular anomaly usually diagnosed in early life, accounting for 5 to 10% of all congenital cardiovascular disorders, but may go unnoticed well until adulthood [7]. Diagnosis is normally based on clinical suspicion and physical findings [8]. Features include hypertension in a young age that does not respond to antihypertensives while physical findings include the difference in blood pressure between the lower and upper limbs, radial-femoral delay and a systolic murmur over the thoracic spine. Other features can include bicuspid aortic valve, systolic ejection sound and/or murmur and neurological manifestations. Prognosis and survival depend on patient's age and disease severity and at the time of intervention. Other known complications are aortic rupture/dissection, concomitant aortic valve disease, coronary artery disease, infective endarteritis/endocarditis, heart failure, or cerebral hemorrhage [8,9]. It is unfortunate that in this case failure in performing a thorough physical examination in lower level facilities led to a delay in making a correct diagnosis and hence the complications. Treatment consists of management of hypertension, of which, angiotensin receptor blockers or angiotensin converting enzyme inhibitors, beta-blockers being the first line drugs. Presence of a peak-to-peak coarctation gradient of at least 20 mm Hg or peak-to-peak coarctation gradient below 20 mm Hg in the presence of anatomic imaging evidence of significant coarctation with radiologic evidence of significant collateral flow are recommendations for interventional and surgical treatment for coarctation lesions [8].
The other challenge in the management of this case is to discern whether to manage the aneurysm first, which is big (measuring 7�mm) and can rupture anytime, or the coarctation. We propose that the patient should first undergo a percutaneous angioplasty to relieve the pressure, which will then also help with the aneurysm, since the higher the pressure, the more the chances of the aneurysm to rupture. A digital subtractive angiography should then follow to assess for other possible aneurysms not seen on Computed Tomography (CT) brain, followed with basilar tip aneurysm embolization and stenting. The last thing will be placing a stent on the aortic coarctation. Since the procedure is expensive, the patient is un-insured, and equipment´s for the procedure is not available in our setting, it is being proposed that he secures Government´s support to enable him to travel to abroad for further management. We pray and hope that the COVID-19 pandemic continues to be controlled to allow for his travel.
In conclusion, this interesting case emphasizes the importance for doctors at all levels of health facilities to always take into consideration the possibility of secondary hypertension in young patients who presents with refractory hypertension, and that a correct physical examination must be conducted. In addition, challenging management issues in are source-constrained setting and the COVID-19 pandemic have been highlighted.
The authors declare no competing interests.
Author´s contribution MPM, RM, ZN, JI and HM admitted the patient and were his attending physicians in the ward. AQ provided his expert opinion in the management of this patient. MB guided the preparation of the manuscript. All authors read and approved the manuscript.
The authors acknowledge the cooperation they got from the patient.
Figure 1: (A,B,C) CT brain with contrast (on different views; left, middle, right) showing basilar tip aneurysm (bold arrow) arising at the tip of basilar artery (arrow), posterior cerebral arteries (PCA) are seen on each side of the aneurysm
Figure 2: chest X-ray revealing marked rib-notching (arrows)
Figure 3: (A,B,C,D) CTA showing coarctation of aorta below the origin of the left subclavian artery with severe stenosis (bold arrow) on different image views; cross-section (upper left), sagittal (lower left), three-dimensional sagittal (middle) and coronal (right)
Figure 4: (A,B) three-dimensional CTA (left and right) showing collateral vessels bypassing the stenotic segment of aorta to perfuse areas distal to the lesion. Note the tortuosity of the collateral vessels (arrows)
- Iuliano L, Micheletta F, Natoli S, Tramaglino L, Greco C, Modesti PA. Aortic coarctation in the elderly: how many errors lie behind an unexpected diagnosis. Intern Emerg Med. 2007;2(3):207-9. PubMed | Google Scholar
- Tanous D, Bensona LN, Horlick EM. Coarctation of the aorta: evaluation and management. Curr Opin Cardiol. 2009;24(6):509-15. PubMed | Google Scholar
- Doshi AR. Coarctation of aorta-management options and decision making. Pediatr Ther. 2012;01(S5). Google Scholar
- Nguyen L, Cook SC. Coarctation of the aorta; strategies for improving outcomes. Cardiol Clin. 2015;33(4):521-30. PubMed | Google Scholar
- Singer MI, Rowen M, Dorsey TJ. Transluminal aortic balloon angioplasty for coarctation of the aorta in the newborn. Am Heart J. 1982;103(1):131-2. PubMed | Google Scholar
- O´Laughlin MP, Perry SB, Lock JE, Mullins CE. Use of endovascular stents in congenital heart disease. Circulation. 1991;83(6):1923-39. PubMed | Google Scholar
- Grech V. Diagnostic and surgical trends, and epidemiology of coarctation of the aorta in a population-based study. Int J Cardiol. 1999;68(2):197-202. PubMed | Google Scholar
- Bhatt AB, Foster E, Kuehl K, Alpert J, Brabeck S, Crumb S et al. Congenital heart disease in the older adult: a scientific statement from the American heart association. Circulation. 2015 May 26;131(21):1884-931. PubMed | Google Scholar
- Jenkins NP, Ward C. Coarctation of the aorta: Natural history and outcome after surgical treatment. QJM - Mon J Assoc Physicians. 1999;92(7):365-71. PubMed | Google Scholar